Back to the Wards from Maternity Leave as an IMG
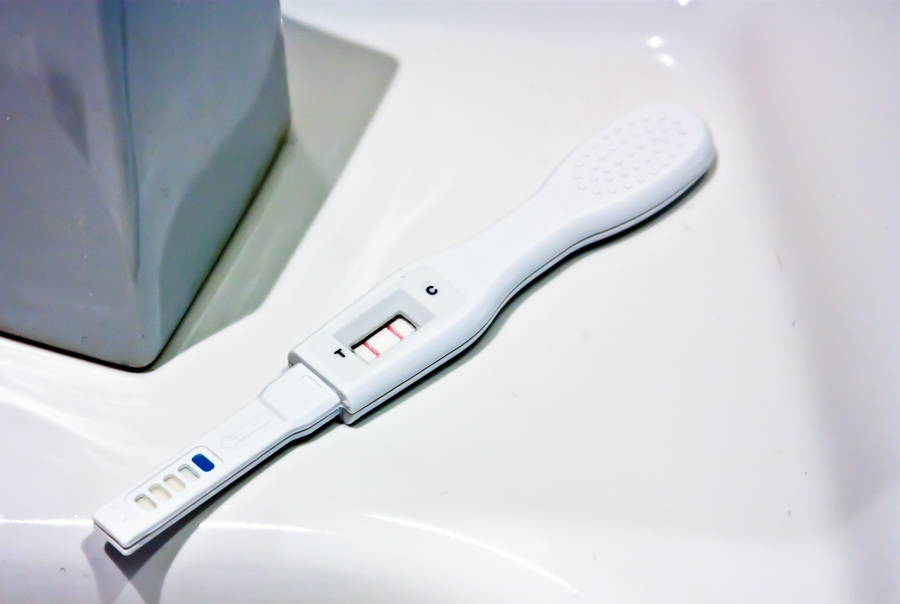
A few months have passed since I wrote my last column article, so now it’s time to get back into it. What has happened in the meantime? Well, I had baby #2, which meant I was lucky enough to take seven weeks of maternity leave from residency.